Leukocytes and PRP
Understanding Leukocyte-Rich vs. Leukocyte-Poor PRP
The optimal leukocyte concentration in platelet-rich plasma (PRP) remains an area of active discussion within regenerative medicine. While published research continues to evolve, Alocuro’s system gives clinicians the flexibility to prepare leukocyte-rich, leukocyte-reduced, or baseline leukocyte PRP from a single device, allowing protocols to be adapted to each clinical application.
How Alocuro System Enables Precision PRP
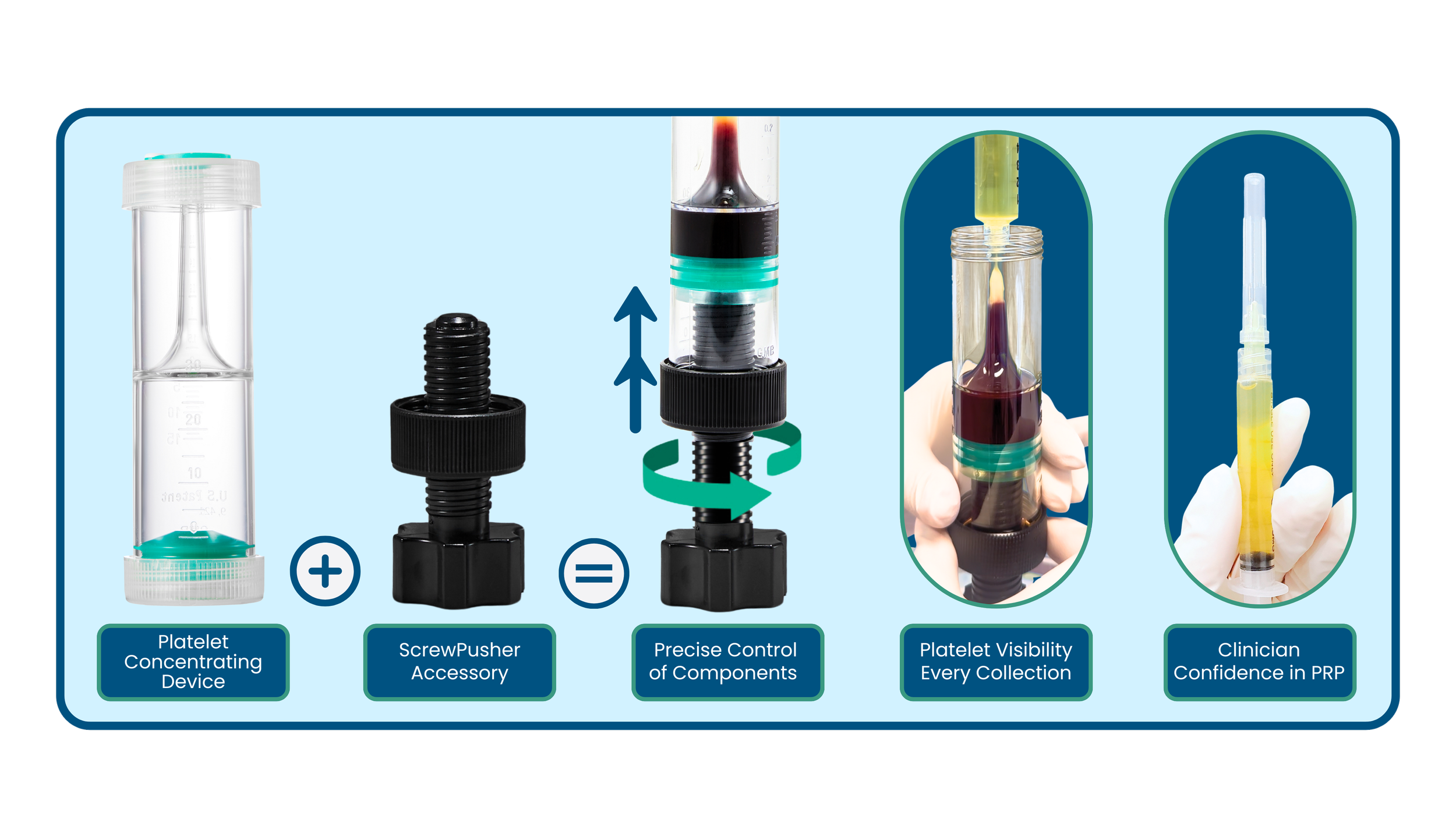
With Alocuro’s PRO-PRP system, practitioners can precisely tailor each PRP preparation to the clinical indication and tissue biology by use of the patented ‘screwpusher’ accessory. The system’s unique flexibility allows adjustment of leukocyte inclusion according to the clinical goal.
This level of control enables clinicians to:
Adjust leukocyte inclusion based on indication and tissue biology
Avoid unnecessary inflammation in joints, and chronic tendon conditions
Deliver consistent, evidence-based outcomes using repeatable protocols
In regenerative medicine, customisation is essential. Alocuro makes it simple, allowing practitioners to deliver biologically appropriate PRP for every patient and every stage of healing.
Cellular Profile: Alocuro’s Leukocyte-Reduced PRP
(From validation conducted by S&N Pathology Clinical Trials Division)
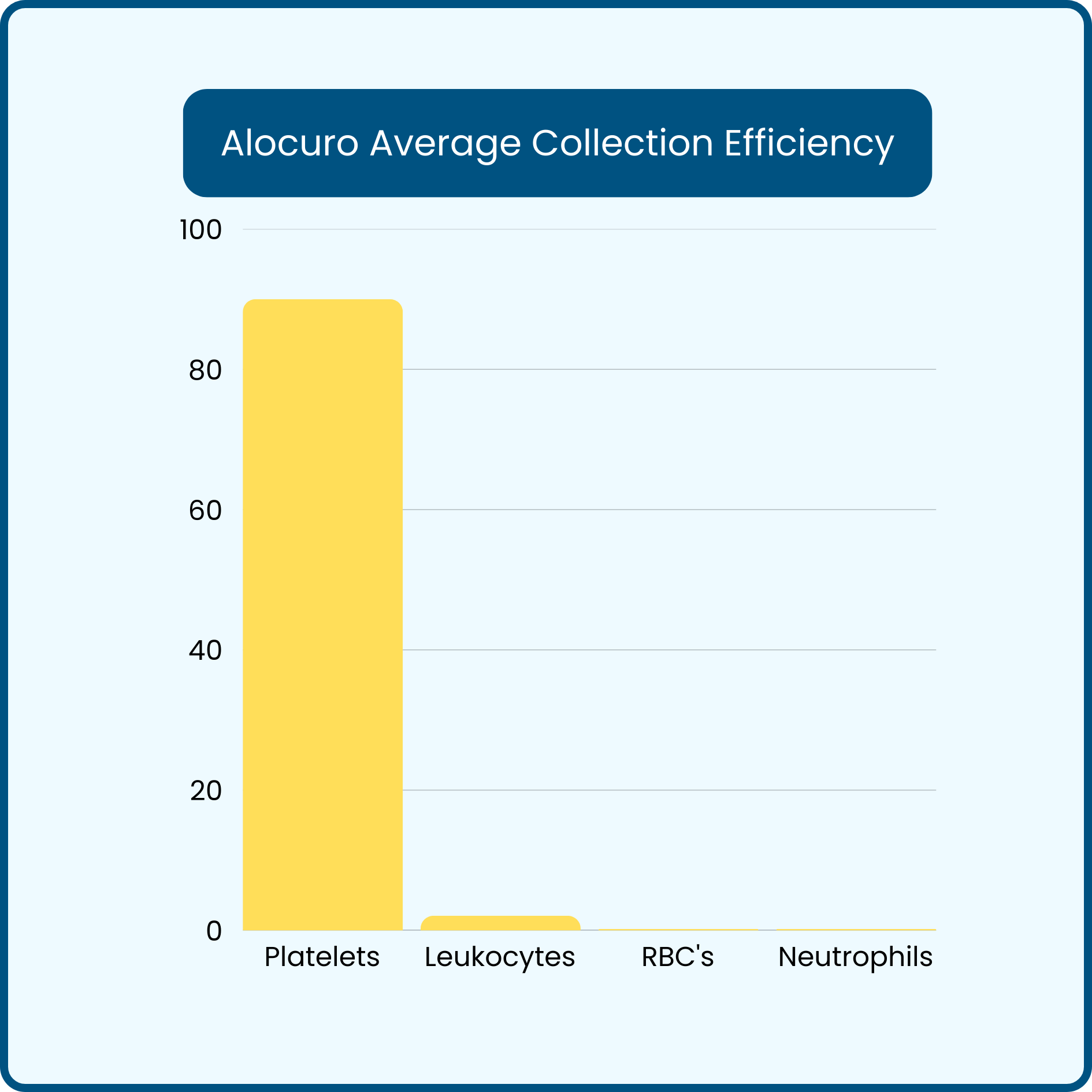
Alocuro Mean Collection Efficiencies:
Platelet collection efficiency: 90%
Total leukocyte collection efficiency: 2.08%
Neutrophil collection efficiency: 0.16%
Red blood cell collection efficiency: 0.19%
These values demonstrate the system’s ability to capture high % platelets with minimal leukocyte & red cells, optimised for intra-articular and chronic tendon PRP applications.
Ongoing Evidence & International Consensus
Despite broad clinical use, no universal standard exists for leukocyte thresholds in PRP. However:
LP-PRP has shown superiority in multiple high-level RCTs for OA
Clinical trial PRP classification now includes leukocyte levels as a defining parameter.
Summary
Alocuro’s dual-configurable system allows clinicians to tailor PRP composition according to the biological needs of the target tissue:
Leukocyte-rich PRP – useful where antimicrobial or early inflammatory activity is desired.
Leukocyte-poor PRP – preferred where chronic inflammation, degenerative pathology, or joint injection is involved.
This flexibility ensures every preparation aligns with evidence-based best practice and procedural precision.
PRP & Joint / Tendon Pathophysiology
Clinical research (e.g. Zhou et al.) shows:
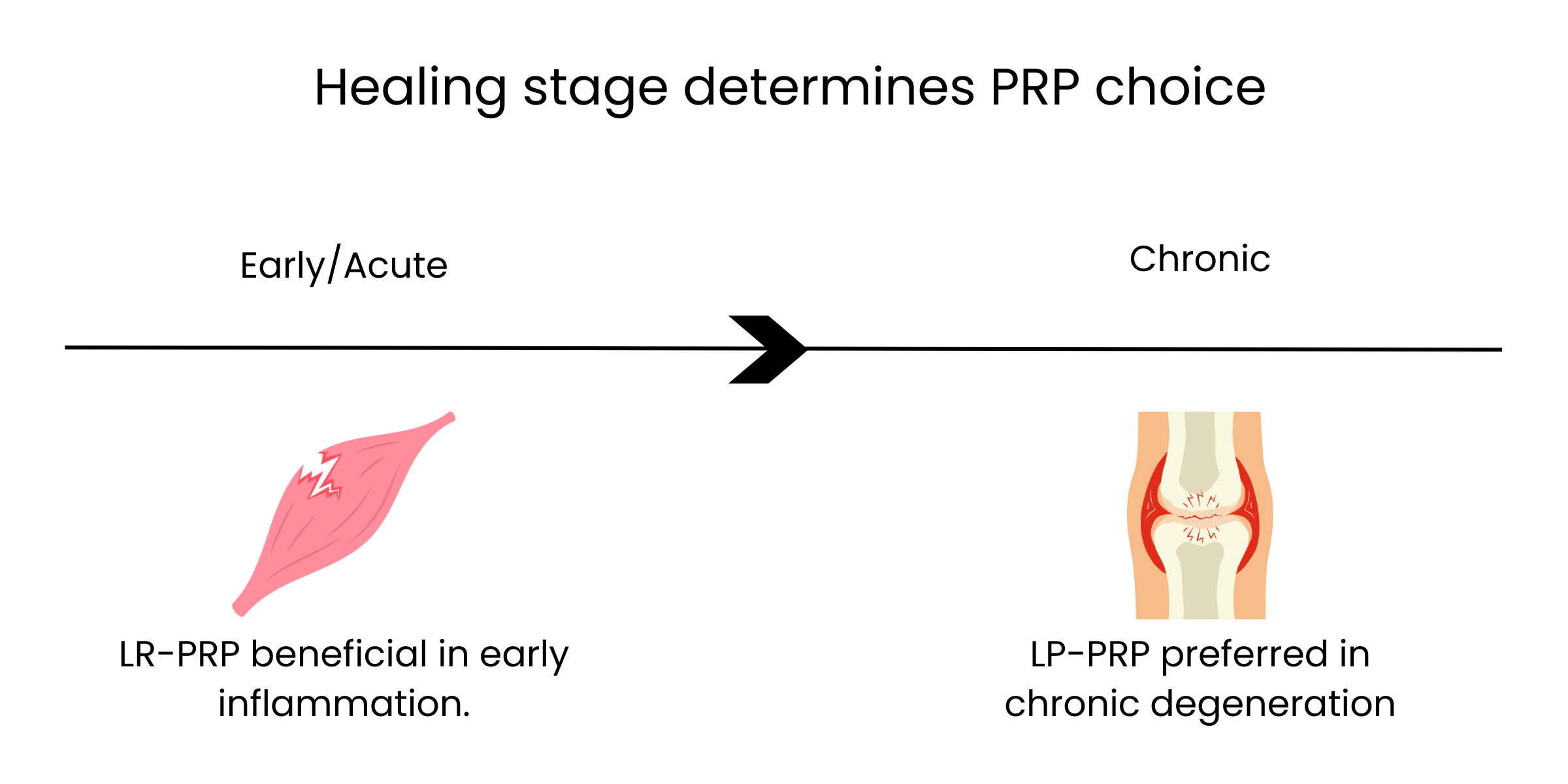
LR-PRP may benefit early inflammatory phases but worsen outcomes in chronic degeneration by stimulating MMPs and IL-6.
LP-PRP is typically chosen for chronic tendon pathology or intra-articular applications where excessive inflammation is counterproductive.
Scar formation risk may increase with high-leukocyte PRP in young tendons during acute repair phase.
PRP type +/- leukocytes is determined on timing after injury and stage of healing.
